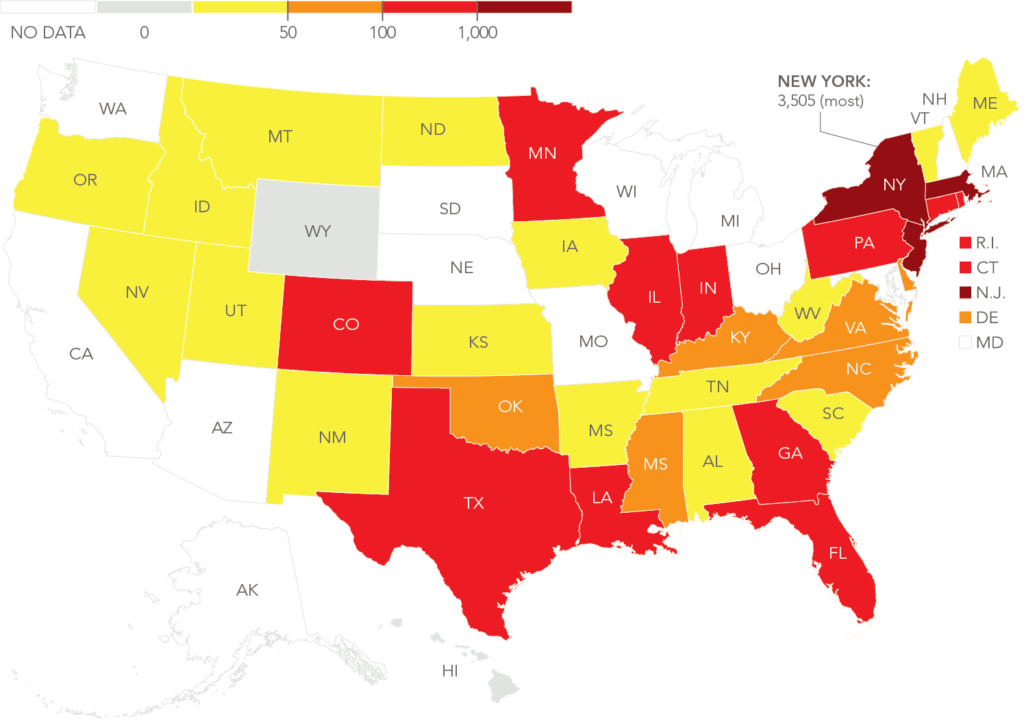
According to a recent Wall Street Journal article and survey, there are at least 10,700 Coronavirus deaths in U.S. nursing homes and long-term care facilities among more than 35 states that either report data online or responded to requests for information. The virus has hit at least 4,800 facilities and the number of people infected, including residents and staff, totals more than 56,000¹.
We know the elder population is extremely vulnerable to this pandemic. Protecting them, as well as those living in nursing homes and long-term care settings, is a matter of growing public concern. More than 2.1 million seniors live in nursing home, skilled nursing and residential care facilities. The realities are these:
- Most who live in residential care settings require health assistance.
- Half are totally dependent on Medicare and social security to cover their long-term care costs.
- Margins in senior care facilities are shrinking.
- Demand for facility-based senior care services is growing.
Facility-based senior and long-term care is an opportunity for innovation and growth. From considering where sanitizer stations and handwashing sinks are placed, to how HVAC systems could be designed in the future to prevent the spread of airborne contaminants, public attention to coronavirus-related infection and death rates will continue. How a facility operates, the infection controls that are in place, and how the physical facilities contribute to resident and staff safety are more critical than ever before.
Every senior care operator should assess the degree of infection-related risks their physical facility, frontline staffing and clinical practices expose. All are essential. And many are paying attention.
In addition to following CDC guidelines, ERDMAN partner Solvere Living, based in St. Petersburg, FL, offered the following as an added measure for their 23 managed communities across the United States.
“As a company, we look at every single resident of every community every day. We are doing resident screenings every day and have added oxygen saturation levels to our screenings where we have had positive COVID identified in a community, as well as increased resident screenings to three times per day. Our SVP of Wellness, a nurse practitioner, and Managing Director of Wellness, an RN, BSN, are reviewing every single resident screening daily for context and intervention needs to ensure we are looking at the whole person and all medical indicators, not just overt COVID symptoms. Additionally, in communities with positive COVID cases, we arm team members with an extra layer of protection, K95 masks, to both residents and to team members.”
If you’d like additional information or for assistance with your risk assessment, contact ERDMAN at info@erdman.com
Facts
- 70% of adults who are 65 years old will require some level of long-term care in their lifetime3
- 67 million family members and friends provide $234 billion in unpaid care for an adult with a chronic illness or disability; 70% of these help with their long-term care costs4
- 1,383,700 receive long-term care in a nursing home, 713,000 live in a residential care community and 273,200 use adult day centers5
- $85,800 is the median overall cost of nursing home services in the United States, ranging from $150,200 in Connecticut to $54,800 in Texas6
- In 2018, the average annual cost for a private patient room in a skilled nursing facility is $100,380 and $89,292 for a semi-private. Both are increasing above inflation: 3.6%/yr. private and 3.2%/yr. semi-private. By contrast, the average annual cost in assisted living was $48,000 (+3.81% from 2017), the average annual cost for adult daycare in 2018 was $18,720, an increase of 1.6%6
CDC Advisory for COVID-19 Response
The CDC issued this advisory to nursing homes and senior living facilities: “Act now to implement ALL COVID-19 preparedness recommendations, even before cases are identified in their community.
Address asymptomatic and pre-symptomatic transmission, implement source control for everyone entering a healthcare facility (e.g., healthcare personnel, patients, visitors), regardless of symptoms.
- Cloth face coverings are not considered personal protective equipment (PPE) because their capability to protect healthcare personnel (HCP) is unknown. Facemasks, if available, should be reserved for Health Care Providers.
- For visitors and residents, a cloth face covering may be appropriate. If a visitor or resident arrives to the facility without a cloth face covering, a facemask may be used for source control if supplies are available.
Dedicate an area of the facility to care for residents with suspected or confirmed COVID-19; consider creating a staffing plan for that specific location.”2
- “Coronavirus Deaths in U.S. Nursing, Long-Term Care Facilities Top 10,000”, Wall Street Journal, April 22, 2020 https://www.wsj.com/articles/coronavirus-deaths-in-u-s-nursing-long-term-care-facilities-top-10-000-11587586237?ns=prod/accounts-wsj.
- “Preparing for COVID-19: Long-term Care Facilities, Nursing Homes” Center for Disease Control and Prevention cdc.gov/coronavirus/2019-ncov/hcp/nursing-home-long-term-care.html.
- Johnson, R. W. (2017). What Is the Lifetime Risk of Needing and Receiving Long-Term Services and Supports?. Washington, DC: The Urban Institute. https://aspe.hhs.gov/basic-report/what-lifetime-risk-needing-and-receiving-long-term-services-and-supports.
- SC Reinhard, LF Feinberg, R Choula, A Houser – Insight on the Issues, 2015 – Valuing the Invaluable, aarp.org, https://www.aarp.org/content/dam/aarp/ ppi/2015/valuing-the-invaluable-2015-update-new.pdf.
- Harris-Kojetin, L. D., Sengupta, M., Lendon, J. P., Rome, V., Valverde, R., & Caffrey, C. (2019). Long-term care providers and services users in the United States, 2015-2016. https://www.cdc.gov/nchs/data/series/sr_03/sr03_43-508.pdf.
- Langdon, Scott (2020). “101 Long Term Care Statistics, Data & Facts [Updated for 2020]”, Money Task Force. https://www.moneytaskforce.com/money/ long-term-care-statistics/.